Medical Tourism Blog
Prostate Disease - What Is It? And How Can it be Treated? with Dr. Sin
Table of contents
- Understanding the Prostate (and Where It Sits)
- What the Prostate Actually Does
- The Three Main Prostate Conditions Men Hear About
- Why Prostate Disease Isn’t Always Straightforward
- Prostatitis: Matching Treatment to the Cause
- Chronic Non-Bacterial Prostatitis: When Pelvic Tension Matters
- BPH (Enlarged Prostate): Why Symptoms Don’t Always Match Size
- Why Diagnosis Comes First (Before Any “Best Treatment”)
- Conclusion: A Clearer Way to Think About Prostate Disease
- More about Yezak Urology
Considering treatment in Korea? Everything you need to know e.g. — how to avoid scams, visas, interpreters, recovery tips — in our Medical Tourism Master Guide. Plan with confidence in minutes, not weeks!
Disclaimer: The following is a guest post. The information and opinions expressed are not of koreaclinicguide.com but of Yezak Urology
Understanding the Prostate (and Where It Sits)
A lot of men hear the word “prostate” but aren’t quite sure what it is or where it’s located. I like to explain it with a simple picture in mind: you have the bladder, and you have the urethra—the tube urine flows through. In men, because there’s a penis, the urethra travels a longer distance from the bladder, roughly about 25 centimeters.

Right at the point where the bladder connects to the urethra, there’s a small structure that wraps around the urethra like a ring. That ring-like structure is the prostate. In most cases, it sits deep in the perineum. This location matters, because when the prostate changes—through inflammation, enlargement, or other disease—it can directly affect the urethra and, in turn, urination.
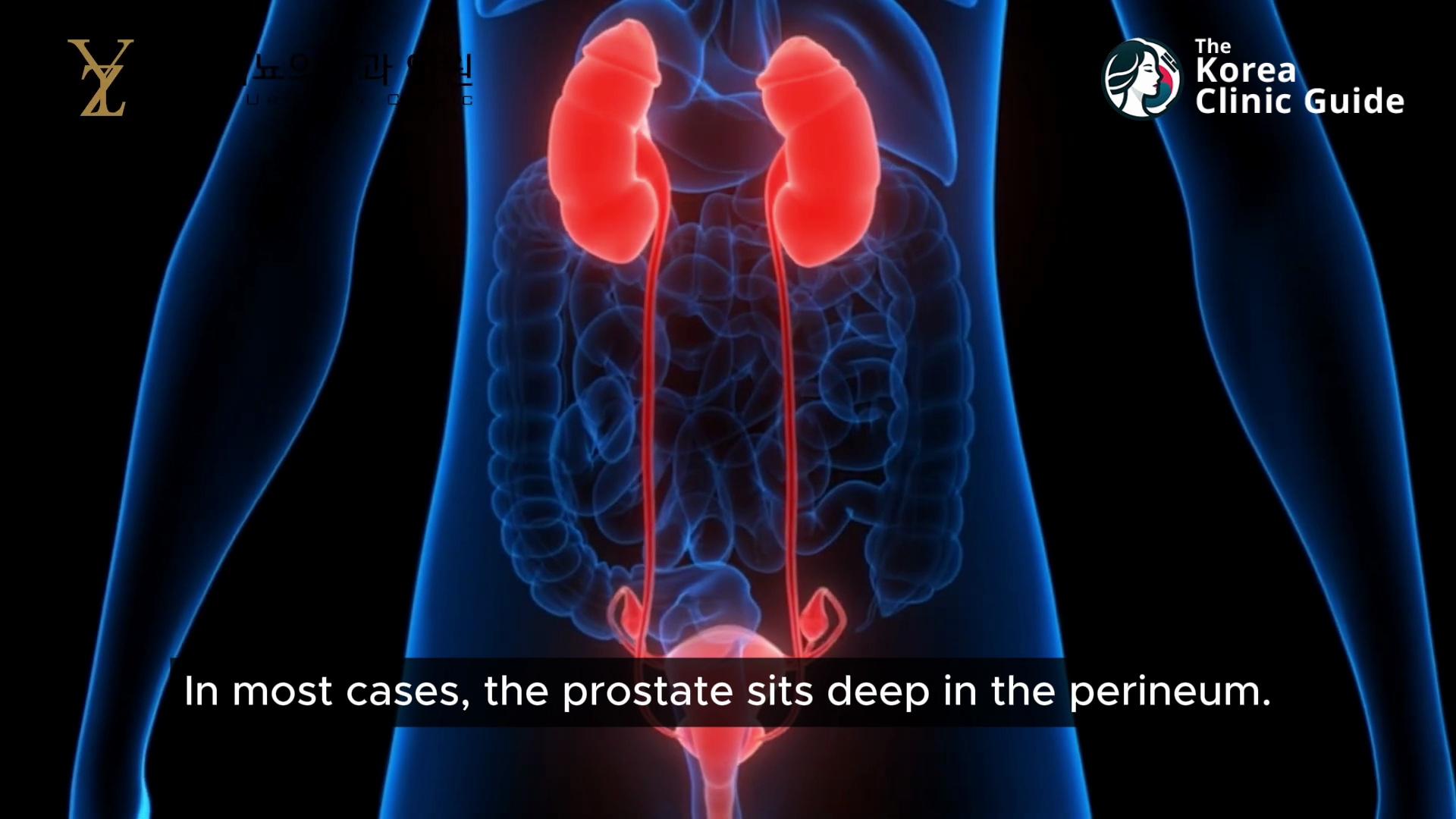
What the Prostate Actually Does
The prostate is not only involved in urination; it’s also a reproductive organ. When a man ejaculates, fluid from the seminal vesicles (which are behind the prostate) mixes with prostatic fluid. Together, these fluids make up most of the semen. That’s why I describe the prostate as a male organ with two key roles: it influences how you urinate, and it contributes to reproduction.
Understanding those two roles helps make sense of why prostate problems can show up as urinary symptoms, pelvic discomfort, sexual changes, or a mix of all three.
The Three Main Prostate Conditions Men Hear About
There are a number of different conditions that can affect the prostate, but three names come up again and again.
First, if the prostate becomes inflamed, that’s called prostatitis. Second, if it enlarges, that’s benign prostatic hyperplasia (BPH). Third, if a cancer develops in the prostate, that’s prostate cancer.
Even though those labels sound straightforward, prostate conditions are often not “one-size-fits-all.” In real life, these conditions can be complex, and the details matter—especially when it comes to choosing the right treatment.
Why Prostate Disease Isn’t Always Straightforward
One of the biggest misunderstandings I see is the idea that every case of prostatitis is the same, or every case of BPH is the same. If you look more closely at prostatitis and BPH, there are actually many subtypes and patterns.
With prostatitis, for example, the approach can differ depending on whether it’s acute or chronic, and whether it’s bacterial inflammation or non-bacterial inflammation. Those distinctions change what we’re trying to treat. Are we trying to eliminate bacteria? Are we trying to calm inflammation and pain? Are we trying to reduce pelvic tension and nerve sensitivity? These are not minor differences—they guide the entire plan.
In chronic, non-bacterial prostatitis, sometimes the problem is not an infection at all. In some cases, the pelvic area can become overly tense, and when that tension persists, the body and nerves can become very sensitive too. When that’s happening, treating it like a simple infection won’t address what’s really driving the symptoms.
With BPH, it’s also not always as simple as “bigger prostate equals worse symptoms.” BPH, in a basic sense, is the prostate getting larger, but symptom severity can be surprising. Some people have significant urinary symptoms even when the prostate isn’t actually that big. Others have very enlarged prostates with hardly any symptoms. That’s why I encourage men not to rely on assumptions and instead talk through their specific pattern with a physician.
Prostatitis: Matching Treatment to the Cause
When people ask me, “What are the treatments for prostatitis?” it can be hard to answer in a single sentence—because the first step is an accurate diagnosis. Treatment depends heavily on whether the prostatitis is bacterial or not.
If prostatitis is caused by bacteria, the goal is clear: eliminate the bacteria. In that situation, antibiotics are usually the first thing to consider, because we’re targeting an infection.
But prostatitis care often isn’t only about addressing the cause. It’s also about controlling the symptoms that make daily life difficult. To manage pain from prostatitis, pain relievers may be used. And for the urinary symptoms that can happen when inflammation makes the prostate swell—especially because the prostate wraps around the urethra—medications that relax and open up the prostatic urethra can also play a role as part of treatment.
In other words, prostatitis treatment frequently has two parallel goals: addressing the underlying driver (such as bacteria when present) and improving comfort and urinary flow while the prostate is irritated and sensitive.
Chronic Non-Bacterial Prostatitis: When Pelvic Tension Matters
In chronic, non-bacterial prostatitis, I pay close attention to the possibility that pelvic tension is contributing to symptoms. If the pelvic area is overly tense, it can keep the region irritated and can make the nerves more reactive. That sensitivity can amplify discomfort and create a cycle that’s hard to break if we only focus on infection.
In those cases, exercises that help relax the pelvic floor can be helpful. In men, this pelvic floor area is the region between the scrotum and the anus. People often recognize the term “Kegel,” but the key here is the concept of relaxation-focused pelvic floor control, not just strengthening. The aim is to reduce chronic tightness and calm the area so the body isn’t constantly bracing.

This is one reason I emphasize classification and careful evaluation: when the mechanism is tension and sensitivity rather than infection, the strategy naturally shifts.
BPH (Enlarged Prostate): Why Symptoms Don’t Always Match Size
BPH is commonly described as “the prostate getting larger,” and that’s true in a general sense. But the lived experience of BPH varies widely.
Some men have bothersome urinary symptoms—like difficulty urinating or changes in flow—even when imaging or examination suggests the prostate isn’t dramatically enlarged. Others have very enlarged prostates with minimal symptoms. That mismatch is exactly why it’s best to sit down with your doctor and talk through what you’re feeling, rather than trying to self-diagnose based on size alone.
The most important practical point is this: BPH is not just a measurement. It’s a condition that has to be understood in the context of symptoms, urinary function, and how much it affects quality of life.
Why Diagnosis Comes First (Before Any “Best Treatment”)
If you ask, “What are the treatments for prostatitis?” or “What are the treatments for BPH?” I understand the desire for a quick answer. But the truth is that prostate disease is rarely something we should treat based on a label alone.
Before choosing a treatment plan, I want to know how the condition is classified. Is prostatitis bacterial or non-bacterial? Is it acute or chronic? Are urinary symptoms coming from swelling and inflammation, or from functional narrowing where relaxing the prostatic urethra would help? Is pelvic floor tension contributing? With BPH, are symptoms actually coming from obstruction, irritation, or another overlapping issue?
Once we know what we’re dealing with, then we can choose a plan that makes sense—whether that means antibiotics for bacterial prostatitis, symptom-focused medications, pain management, or relaxation-focused pelvic floor strategies.
Conclusion: A Clearer Way to Think About Prostate Disease
The prostate is a small ring-like gland at the junction of the bladder and urethra, but it has an outsized impact on both urination and reproduction. Because of its location and function, prostate disease can show up in multiple ways—and the same diagnosis name can still represent several different subtypes.
In my view, the most helpful approach is to start with clarity: understand whether you’re dealing with inflammation, enlargement, infection, tension-related sensitivity, or a combination. From there, treatment becomes much more logical—whether it involves antibiotics for bacterial prostatitis, medications to reduce pain and improve urinary flow, or pelvic floor relaxation techniques in chronic non-bacterial cases. When men stop guessing and start with an accurate diagnosis, they usually get to better, more targeted relief.
More about Yezak Urology
In Seoul’s Apgujeong, Yezak Urology Clinic stands out as one of the city’s largest urology centers and a dedicated men’s health hub for patients seeking thorough evaluation and treatment of prostate-related concerns such as frequent urination, weak stream, nocturia, pelvic discomfort, or prostate inflammation, with care plans that address underlying causes and long-term management. Backed by more than 20 years of experience in male-focused urology and equipped with the latest advanced technology and robust safety systems, the clinic offers a multi-specialist approach that can connect prostate symptom care with broader men’s health needs, including erectile dysfunction and hormonal changes that often coexist. Led by a renowned urology specialist who developed the innovative 5-Point Fixed Permanent Penile Lengthening Surgery, Yezak is distinguished by deep surgical expertise and meticulous, evidence-informed protocols across both surgical and non-surgical treatments, providing patients with comprehensive, privacy-centered care in a high-capacity Korean urology setting.
Find more about this clinic here: Yezak Urology















